Cardiovascular examination

Check out the basics of examination
General Examination
Say: "patient looks generally well, pink on air, no evidence of dyspnoea or tachypnoea and no obvious scars, deformity or other abnormality."
With cardiovascular, look if the patient is short of breath, oxygen, sitting up with like twenty pillows (possibly heart failure).
Hands
Basically, you need to say maybe two or three of these things. Pick ones you know about and you can say "stigmata of endocarditis" but if you do say it, know some. Here are a few you can pick from:
Signs: temperature (compare with forearm using backs of your hands), tremor (get patient to hold out hands with straight arms - both hyperthyroidism); tendon xanthoma (yellow deposit of extensor surface of wrist - type II hyperlipidaemia); peripheral cyanosis (due to cold, poor circulation); arachnodactyly (abnormally long, slender fingers - Marfan's)
Stigmata of endocarditis (say "stigmata" because it makes you sound clever): nails - finger clubbing, splinter haemorrhages; Osler's nodes (0.5-1 cm red-brown painful subcutaneous papules on fingertips, palmar eminences); Janeway lesions (flat red macules, on the thenar and hypothenar eminences)
Pulse
Report on rate (feel for 10s and multiply by 6) and rhythm (regularly regular, in a normal person). Wait until you get to the carotid before you start commenting on other things.
Check for Radial-radial delay and radiofemoral delay (coarctation of the aorta, before the left subclavian artery in radial-radial)
Check for a collapsing/waterhammer pulse:
- feel the muscle in the forearm
- check the patient has not musculoskeletal problems in the shoulder or arm
- lift the arm
- if a pulse is felt, the patient has a collapsing/waterhammer pulse
- say: "no waterhammer pulse present"
(Caused by: )
Face
- General: malar flush (thin face, purple cheeks - mitral stenosis); any facies that are characteristic of specific diseases - Cushing's (mooooooooooooooonface, also with hypertension), acromegaly (also has hypertension and CHF)
- Eyes: anaemia (pull down on eyelids, and see if they are pale); xanthelesma (periorbital yellow plaques) - hypercholesterolaemia, DM; corneal arcus - hypercholesterolaemia; Roth spots (red haemorrhage with pale centre on opthalmoscopy) - endocarditis.
- Mouth: central cyanosis in lips and tongue; high arch palate - Marfan's
Neck
- JVP - look for height and character. The internal JVP is between the heads of the sternocleidomastoid muscle. The external JVP is lateral to that same muscle. Say: "looking for any rise in JVP"
- Carotid - inspect for pulsations; palpate for character and volume, auscultate for carotid bruits (aortic stenosis). Say: "looking for pulsations, feeling for pulse character and volume and listening for carotid bruits".
- Tracheal deviation (warn the patient, then put index and ring fingers on the two SCMs and poke either side of the trachea with your middle finger) - penumothorax, lung cancer or other mass. Say: "looking for any tracheal deviation".
Chest
Also known as the precordium, this basically refers to the front of the chest.
Inspect
- Look for: scars, deformity, dressings stitching. Check left axilla for mitral valvotomy scar. Make this really obvious.
- Say: "checking for scars, deformity, visible pulsations or any other abnormalities."
Palpate
- Ask about any tenderness
- Feel for
- Apex beat (put your hand on the left side of the precordiumshould be in the mid-clavicular line, 4th/5th intercostal space) - defined as the most inferolateral point at which the heart can be palpated
- Heaves (put your hand across their chest)
- Parasternal thrills (palpable murmurs - put your hands either sides of the sternum)
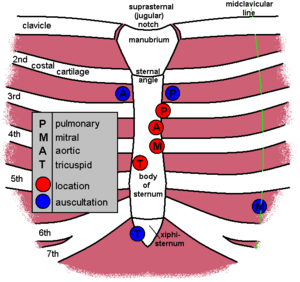
Auscultate
The four main areas to listen to with the diaphragm are:
- Mitral: Left hand side of the sternum at the fourth costal cartilage
- Tricuspid: Right hand side of the sternum at the fourth intercostal space
- Pulmonary: Medial end of the third costal cartilage
- Aortic: Left hand side of the sternum at the third intercostal space
You should also listen to:
- Left axilla in left lateral position (rolled over to the left) with bell
- Mitral area with bell
- Tricupsid area, sitting forward on held inspiration (ask the patient to take a deep breath in, then out and hold it) with diaphragm
- Carotids with bell
Extras
Back
- Inspect: scars, deformity, sacral oedema
- Auscultate: lung bases for crackles, a sign of pulmonary oedema and thus heart failure
Feet
Check for pulmonary oedema - inspect and palpate (comment on whether it's bi/unilateral, how high up it goes and whether it's pitting)
Blood Pressure
Don't forget to say: "I would take a blood pressure reading to complete my examination."