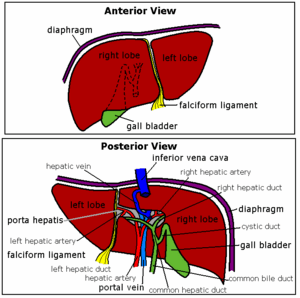
Liver
Structure and Function
Structure
The liver is soft and pliable and situated the upper part of the abdominal cavity, just below ‘t diaphragm. It is found just under the right hand side of the costal margin. The convex upper surface of the liver is moulded to the under surface of the domes of the diagram. The visceral surface is moulded to adjacent viscera and is therefore irregular in shape.
The liver is divided into a large right lobe and a small left lobe, divided by the falciform ligament of the peritoneum. The right lobe is divided into bits by the gall bladder, vena cava and some ligaments; the bits are called the 'quadrate' and 'caudate'. The liver is completely surrounded by a fibrous capsule, partly covered by the peritoneum.
Lobules
The lobes contain thousands of subunits called lobules. Each lobule has a central vein which is a tributary to the hepatic veins. There are portal canals in the spaces between lobes. These contains the portal triad:
- Branches of the portal vein
- Branches of the hepatic artery
- Tributaries of the bile duct
Vessels
The porta hepatis or hilum of the liver is found on the posterioinferior surface and lies between the quadrate and caudate lobes. Attached to upper part of the lesser omentum it contains the:
- Hepatic Ducts (R+L)
- Hepatic Artery (R+L)
- Portal Vein
- Para + sympa nerve fibres
- Lymph nodes (drain liver and gallbladder into coeliac nodes)
Functions
Metabolic processes:
Carbohydrate metabolism:
- Gluconeogenesis (aminos, lactate or glycerol -> glucose)
- Glycogenolysis (glycogen -> glucose)
- Glycogenesis (glucose -> glycogen)
Lipid metabolism:
- Cholesterol synthesis
- Production of triglycerides
Storage:
- Glycogen
- Vitamin B12
- Iron
- Copper
Production and secretion of bile:
- Synthesizes heparin which is an anticoagulant
- Synthesises bile pigments from the haemoglobin of worn out rb corpuscles.
- Secretes bile salts
Other functions
- Breaks down haemoglobin (bile pigments are its metabolites), toxic stuff and some drugs. This sometimes results in toxication, where the metabolite is more toxic than its precursor.
- Converts Ammonia to urea.
- Production of coagulation factors
- In the first 3 months, the liver is the main site of RDC production in the foetus, but by the 42nd the bone marrow has completely taken over.
Arterial and Venous supply
Nervous Supply
Lymph
Liver produce 1/3 to ½ of all body lymph. Lymph vessels in liver -> lymph nodes in porta hepatis -> celiac nodes.
Histology
Clinical conditions
Hepatitus viruses
| Virus | Type of virus | Incubation Period | Illness | Carriers | Serological markers | Patient susceptibility | Transmission |
| HAV | ssRNA enterovirus | 15-40 days | Mild; very low mortality | No | IgM anti-HAV antibody | Young | Faecal-oral |
| HBV | dsDNA hepadnavirus | 50-180 days | Significant risk of chronicity and mortality | Yes | HBsAg, HBeAg | Any age | Blood and blood; needles; venereal. |
| HCV | Ss+RNA | 40-55 | Fluctuating; significant risk of chronicity and mortality | Yes | Anti-HCV antibody, HCV RNA | Any age | Blood and blood products; needles; possibly venereal. |
| HEV | ssRNA virus | 30-50 | No risk of chronicity; high mortality in pregnancy | No | Anti-HEV antibody | Any age | Faecal-oral |
Hepatitis A
- Usually an epidemic.
- Virus excreted in faeces before the symptoms occur.
- Liver damage is direct cytopathic effect – rather than autoimmune.
Hepatitis B
- HBsAG – the Hep B surface antigen sticks to the liver cell surface, thus initiating an immune response, so the liver cell is attacked.
- HBeAG – prescence of this indicates liver disease.
- B goes chronic in 5% of patients
For more, check out the page on Hepatitis B
Hepatitis C
- High mutation rate. These ongoing changes in the virus make it difficult for the immune system to fight it off. For the same reason it is very difficult to develop a vaccine.
- Almost always blood born.
- It becomes chronic in 50-80% of cases, though when so is generally milder than chronic B.
- In chronic, cirrhosis occurs in 20-30%, though primary liver cancer appears to be much less common.
Jaundice
Can be caused by a variety of things:
- Physiological neonatal: relatively common in premature infants. (membrane between the blood and the brain is really thin in babies, so unconjugated bilirubin gets into the brain)
- Structural: Biliary Atresia – where the bile duct fails to develop
- Functional: Congenital metabolic defects involving the liver
Can be classified into 3 types:
Prehepatic
In these there is excess bilirubin from the break down of blood cells – Haemolysis. Because the excess bilirubin is unconjugated (and thus insoluble) it cant be excreted so the bile contains so much bilirubin it puts the person at risk of gall stones.
Intrahepatic
Caused by hepatic disorders such as:
- Acute viral hepatitis
- Cirrhosis
- Drug induced liver injury
- Alcoholic hepatitis
- Intrahepatic bile duct loss
The excess bilirubin is predominantly conjugated (and so soluble), and so is excreted in the urine and causes dark urine. Congenital defect in conjugation/transport/excretion of bilirubin: Gilberts, Crigler-Najjir, and probably other eponymous syndromes such as William-St Hellen’s-Mildred-Chocolate Biscuits-Hot Cross Bun-Fish-!-Hmmm syndrome
Post hepatic
Inteferes with biliarry drainage, the excess conjugated bilirubin produces dark urine and pale stools.
Obstruction to extra hepatic bile ducts:
- Tumour – carcinoma at head of the pancreas compresses the bile duct
- Strictures – post surgery
- Gall stones – usually associated with biliary colic (severe abdominal pain), with a non distendable chronically inflamed gall bladder,
- Congenital biliary atresia