Hyponatraemia: Difference between revisions
Jump to navigation
Jump to search

Kingrajinix (talk | contribs) |
No edit summary |
||
| (10 intermediate revisions by 2 users not shown) | |||
| Line 1: | Line 1: | ||
[[image: | [[image:emptysalt.jpg|right|thumb|200px|This empty salt shaker is suffering from [[hyponatraemia]].]] | ||
===Definition=== | ===Definition=== | ||
[[Serum sodium]]<135mmol/L (<120mmol/L is severe). | [[Serum sodium]]<135mmol/L (<120mmol/L is severe). | ||
===Epidemiology=== | ===Epidemiology=== | ||
[[image:common.jpg]]It is the most common electrolyte abnormality. 4.4% of postoperative patient have it. Almost 100% will have had an operation. | [[image:common.jpg|left]]It is the most common electrolyte abnormality. 4.4% of postoperative patient have it. Almost 100% will have had an operation. | ||
===Pathophysiology=== | ===Pathophysiology=== | ||
In a nutshell:<br> | |||
[[image:lowsodium.jpg|500px]] | |||
====Hypovolaemic==== | ====Hypovolaemic==== | ||
*Kidney problems - [[Addison's]], [[renal failure]], [[acute tubular necrosis]], chronic [[pyelonephritis]], diuretics and others | *'''Kidney problems''' - [[Addison's]], [[renal failure]], [[acute tubular necrosis]], chronic [[pyelonephritis]], diuretics and others | ||
*Non-renal - [[diarrhoea]] and/or [[vomiting]], [[burns]], [[pancreatitis]], [[trauma]], fistula, small [[bowel obstruction]], endurace sport event, heat exposure | *'''Non-renal''' - [[diarrhoea]] and/or [[vomiting]], [[burns]], [[pancreatitis]], [[trauma]], fistula, small [[bowel obstruction]], endurace sport event, heat exposure | ||
====Not hypovolaemic==== | ====Not hypovolaemic==== | ||
*Oedmatous - [[nephrotic syndrome]], [[heart failure]], [[cirrhosis]], [[renal failure]] | *'''Oedmatous''' - [[nephrotic syndrome]], [[heart failure]], [[cirrhosis]], [[renal failure]] | ||
*Normovolaemic - [[SIADH]], water overload, severe [[hypothyroidism]], glucocorticoid deficiency | *'''Normovolaemic''' - [[SIADH]], water overload, severe [[hypothyroidism]], glucocorticoid deficiency | ||
===Clinical Features=== | ===Clinical Features=== | ||
*Neuro - [[headache]], [[decreased level of consciouness]], [[cognitive impairment]], [[personality change]] [[seizure]], brain stem herniation (fixed unilateral dilated pupil, [[coma|decorticate or decerebrate postuiring]], [[respiratory arrest]]) | *Neuro - [[headache]], [[decreased level of consciouness]], [[cognitive impairment]], [[personality change]] [[seizure]], brain stem herniation (fixed unilateral dilated pupil, [[coma|decorticate or decerebrate postuiring]], [[respiratory arrest]]) | ||
| Line 25: | Line 28: | ||
Firstly determine their hydration status. Then the most important things are: | Firstly determine their hydration status. Then the most important things are: | ||
*Urinary sodium | *Urinary sodium | ||
*Urine | *Urine osmolality | ||
The reason being the help to determine which of the [[#Pathophysiology|causes]] is most likely. | The reason being the help to determine which of the [[#Pathophysiology|causes]] is most likely. | ||
In '''hypovolaemia''': | In '''hypovolaemia''': | ||
| Line 35: | Line 38: | ||
===Management=== | ===Management=== | ||
*Hypovolaemia - isotonic saline replacement | |||
*Normovolaemia - '''fluid restrict''' to 500ml/24h. | |||
*Hypervolaemia - '''furosemide''', ACE inhibitors, fluid restrict. | |||
===Prognosis=== | ===Prognosis=== | ||
Latest revision as of 08:46, 23 March 2011

This empty salt shaker is suffering from hyponatraemia.
Definition
Serum sodium<135mmol/L (<120mmol/L is severe).
Epidemiology
It is the most common electrolyte abnormality. 4.4% of postoperative patient have it. Almost 100% will have had an operation.
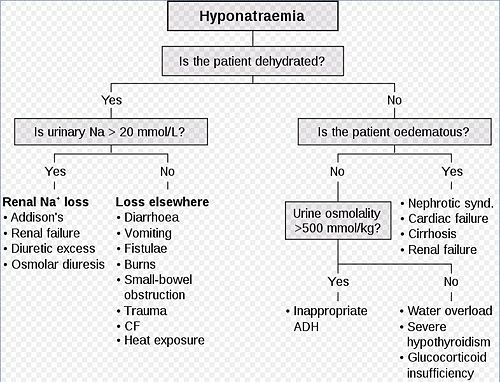
Pathophysiology
Hypovolaemic
- Kidney problems - Addison's, renal failure, acute tubular necrosis, chronic pyelonephritis, diuretics and others
- Non-renal - diarrhoea and/or vomiting, burns, pancreatitis, trauma, fistula, small bowel obstruction, endurace sport event, heat exposure
Not hypovolaemic
- Oedmatous - nephrotic syndrome, heart failure, cirrhosis, renal failure
- Normovolaemic - SIADH, water overload, severe hypothyroidism, glucocorticoid deficiency
Clinical Features
- Neuro - headache, decreased level of consciouness, cognitive impairment, personality change seizure, brain stem herniation (fixed unilateral dilated pupil, decorticate or decerebrate postuiring, respiratory arrest)
- GI - nausea, vomiting
- General - lethargy, muscle cramps and weakness
- If hypovolaemia - dry mucous membranes, tachycardia, reduced skin turgor
- If hypervolaemia - crackles, third heart sound, raised JVP, peripheral oedema, ascites
Investigations
Dehydration
- U+Es are useful for sodium (obviously) but also assessing dehydration (urea and creatinine).
Further diagnosis
Firstly determine their hydration status. Then the most important things are:
- Urinary sodium
- Urine osmolality
The reason being the help to determine which of the causes is most likely. In hypovolaemia:
- Urinary sodium >20mmol/L - renal cause
- Urinary sodium <20mmol/L - non-renal cause
In normovolaemia:
- Urine osmolality >100mOsmol/kg - SIADH
Otherwise, it must be something else. See pathophysiology.
Management
- Hypovolaemia - isotonic saline replacement
- Normovolaemia - fluid restrict to 500ml/24h.
- Hypervolaemia - furosemide, ACE inhibitors, fluid restrict.